Sciatica is a condition in which the sciatic nerve is compressed, causing referral symptoms (often pain or numbness) into the lower extremity. The referral symptoms can be sensory and/or motor depending on whether sensory or motor neurons are compressed

And now for the technical part – empowering you!
The sciatic nerve is formed when the L4, L5, S1, S2, and S3 nerve roots merge in the abdominopelvic cavity. The sciatic nerve exits through the greater sciatic foramen into the posterior pelvis / gluteal region between the piriformis and superior gemellus muscles.
There is a fairly common variation (found in approximately 15% of people) in which part or all of the sciatic nerve exits/pierces through the piriformis muscle itself. The sciatic nerve then travels down the posterior thigh, innervating the musculature of the posterior thigh (hamstrings and posterior head of adductor magnus) along the way.
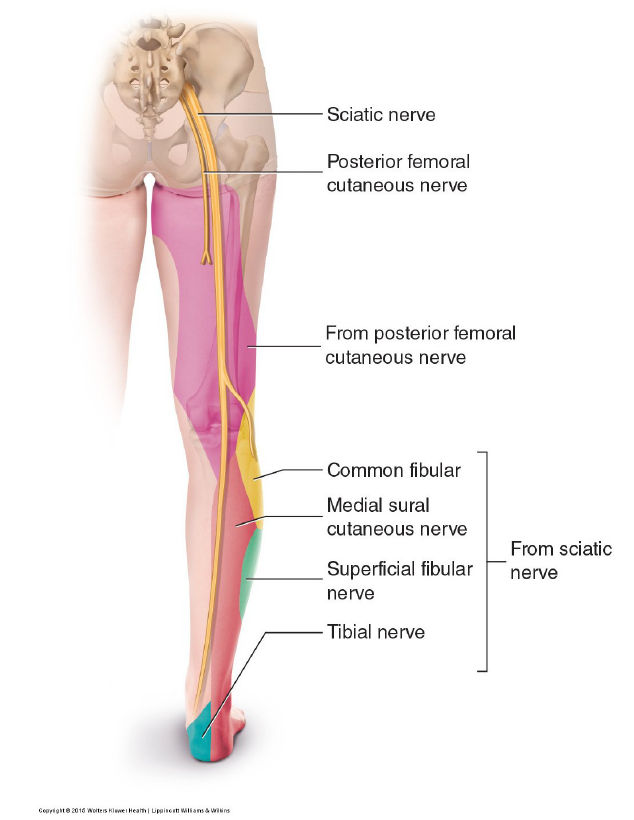
Just proximal to the knee, the sciatic nerve splits into the tibial nerve (L4, L5, S1, S2, and S3) and the common fibular nerve (L4, L5, S1, and S2) (Note: The common fibular nerve used to be called the common peroneal nerve.) The tibial nerve continues down the posterior leg and innervates all the muscles in the superficial and deep posterior compartments of the leg. It then enters the foot posterior to the medial malleolus of the tibia and divides to become the medial and lateral plantar nerves, innervating the plantar intrinsic musculature of the foot.
The common fibular nerve splits to form the superficial and deep fibular nerves (old names: superficial and deep peroneal nerves). The superficial fibular nerve innervates the muscles of the lateral compartment of the leg (fibularis longus and brevis). The deep fibular nerve innervates the muscles of the anterior compartment of the leg (tibialis anterior, extensor hallucis longus, extensor digitorum longus, and fibularis tertius). It then travels into the foot, crossing the ankle joint anteriorly, and innervates the dorsal intrinsic musculature of the foot (extensor hallucis brevis and extensor digitorum brevis).
What does the Sciatic nerve do?

The sciatic nerve provides both motor and sensory innervation. The sciatic nerve and its branches innervate the musculature of the posterior thigh and all musculature distal to the knee joint. Its sensory innervation distribution is to the lateral leg (posterior and anterior
and the entire foot. A dermatomal map can be used to map out where the sensory innervation is for each of the spinal nerve roots of the sciatic nerve.
Causes of sciatica
Given that sciatica is caused by compression of the sciatic nerve, anything that can compress the sciatic nerve can theoretically cause sciatica. The two most common causes of sciatica occur at the spine and are a pathologic disc (bulging or herniated) or an osteoarthritic bone spur.
These space-occupying (nerve impingement) lesions can compress a nerve root of the sciatic nerve as it passes through the intervertebral foramen (IVF). The term lateral stenosis is used to describe stenosis within the IVF.
A pathologic disc can also cause direct compression against the spinal cord in the central canal. Stenosis within the central canal is termed central canal stenosis. The exact symptoms that the client/patient experiences will depend upon which neurons of the spinal cord or nerve roots are compressed.
Another fairly common cause of sciatica is piriformis syndrome in which a tight piriformis compresses against the sciatic nerve. This compression can occur regardless of the sciatic nerve’s presentation in the gluteal region.
Therefore, anything that tends to increase the baseline tone of the piriformis can contribute toward piriformis syndrome as the cause of sciatica. The baseline tone of the piriformis will increase with all postures and movement patterns that place an excessive demand upon lateral (external) rotation of the thigh at the hip joint.
A number of other factors can contribute to sciatica. Swelling often accompanies a pathologic disc and can further the sciatic compression within the IVF or central canal. Ligament hypertrophy within the central canal is another fairly common cause of sciatica; this usually occurs in elderly people. Although not very common, a cyst or tumor could potentially cause compress the sciatic nerve and cause sciatica with its characteristic referral symptoms. Even trauma to the sciatic nerve in the gluteal region or lower extremity can cause sciatica.
Signs and symptoms of sciatica
Compression upon the sciatic nerve can decrease its transmission by partially or entirely blocking the ability of neurons to carry their signals. This can result in numbness or decreased sensation (hypesthesia) within the innervation region of the sciatic nerve (note: the term “paresthesia” is used to denote any altered sensation). In addition to symptoms within the innervation region of the sciatic nerve, pain along the course of the sciatic nerve within the buttock or posterior thigh is also possible. Indeed, pain shooting down the posterior thigh is a fairly common symptom for clients/patients experiencing sciatica.
Decreased signal conduction within the motor neurons of the sciatic nerve can result in weakness of the musculature innervated by the sciatic nerve. A very common sign of sciatica is “foot drop.” The term foot drop describes the characteristic manner in which the foot drops against the ground during the gait cycle because of the weakness of ankle joint dorsiflexors. When weakened, dorsiflexion musculature is not strong enough to eccentrically contract to gracefully control the descent of the foot as we step forward. Therefore, instead of lowering against the ground with control, the foot drops against the ground, often making a slapping noise.
Conversely, compression can increase nerve signal conductance if the compression irritates the neuron, triggering action potentials. If sensory neurons are irritated, the client/patient might have tingling, increased sensitivity, or pain (hyperesthesia) within the innervation region of the sciatic nerve.
If sciatic motor neurons are irritated, twitching or spasming of the associated musculature might occur. The exact location of the symptoms of sciatica would be determined by which neurons are compressed; in other words, which nerve root level is affected (from L4 to S3), and whether they are sensory or motor neurons.
Given the location of the sciatic nerve and its wide expanse of sensory distribution, the symptoms could range from sharp pain in the posterior thigh, to burning discomfort in the lateral leg, to numbness in the big toe. Similarly, motor symptoms can potentially range from twitching or spasming of the hamstrings, to weakness of musculature of the foot or toes. If sciatica is caused by a space-occupying lesion (nerve compression) within the intervertebral foramen (IVF), whether it is a pathologic disc or an osteoarthritic bone spur, then anything that compresses and narrows the IVF will likely increase the symptoms of sciatica.
For this reason, positions of weight bearing (sitting and standing) often increase the symptomology of sciatica. Spinal extension can also be problematic because it decreases the size of the IVFs, thereby likely increasing compression upon the nerve roots. If the cause of the sciatica is a pathologic disc, then spinal flexion can also be difficult for some clients/patients because it compresses the anterior disc, driving the nucleus pulposus posteriorly against the damaged annular fibers, thereby increasing the bulging/herniation pressure against the nerve.
Massage West Lothian & Expert Physiotherapy – The Right Assessments!
In a sense, sciatica is not a condition but rather a sign of another condition: a space-occupying (nerve compression) condition that is compressing the sciatic nerve. Therefore, successful assessment/diagnosis of sciatica depends upon successfully assessing the underlying cause of the sciatic nerve compression.

Treatment
It is difficult to state what manual therapy treatment techniques will necessarily be beneficial for sciatica because, as stated, sciatica describes the symptom (compression of the sciatic nerve), not the underlying mechanism of the condition itself. Therefore, it is necessary to determine what condition is causing the sciatic nerve compression and address that. If the cause is a pathologic disc, then addressing factors that affect disc compression is appropriate.
If the cause is osteoarthritis/degenerative joint disease, then addressing this condition is required. And, of course, if the cause is piriformis syndrome, then the piriformis needs to be treated. Once determined, the tools that are at the disposal of the manual therapist are essentially soft tissue manipulation (massage), hydrotherapy (hot and cold), stretching, and joint mobilization (arthrofascial stretching).

Massage Bathgate – Leading the way in Clinical Massage & Physiotherapy
massage west lothian
massage bathgate
physiotherapy west lothian
physiotherapy west lothian



